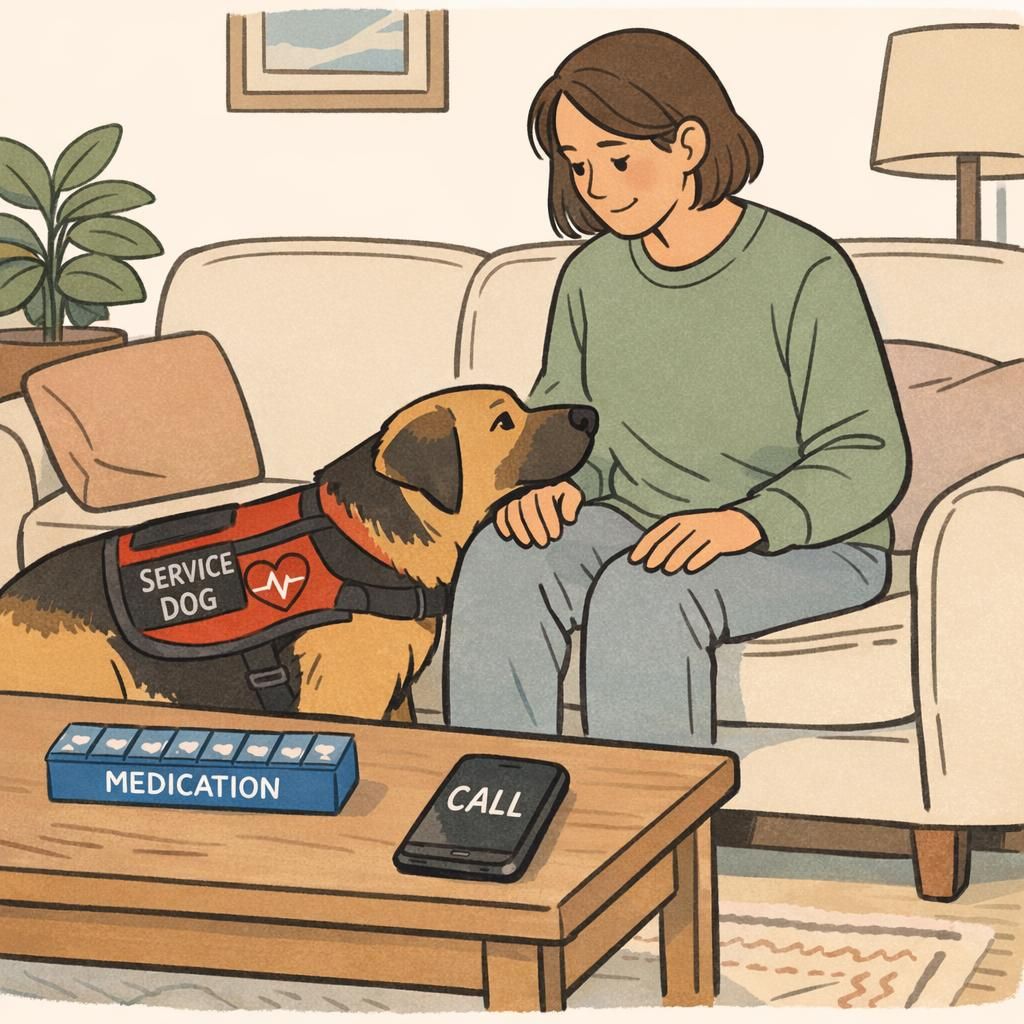
A cardiac alert dog (sometimes called a heart alert dog) is a type of medical alert service dog trained to recognize signs that a person’s body is shifting toward a symptom episode related to heart rate or blood pressure changes. In everyday terms, these dogs help by noticing “something is different” in their handler’s body or behavior and then performing a trained alert so the person can take practical safety steps.
People seek cardiac alert support for a wide range of day-to-day challenges, including episodes that may involve rapid or irregular heart rate, sudden blood pressure drops, dizziness, lightheadedness, weakness, or fainting risk. Some handlers live with predictable patterns (for example, symptoms after standing up quickly), while others experience changes that feel random. A well-matched dog can become an added layer of support—especially when symptoms are subtle at first and escalate quickly.
It’s also important to set realistic expectations. “Cardiac alert dog” is a helpful label, but it isn’t a one-size-fits-all job description. One handler may need early alerts before dizziness hits, while another may rely more on response tasks after symptoms begin (like help-seeking or medication retrieval). Many teams combine alert behaviors with calm grounding support, structured routines, and a safety plan created alongside a clinician’s guidance.
In daily life, a cardiac alert often looks simple: a dog nudges, paws, licks, stares intently, blocks forward movement, or stays glued to the handler’s side. The key is that the behavior is noticeable, repeatable, and clearly different from the dog’s normal “hanging out” mode. Over time, handlers learn their dog’s alert style and what it usually means for their body.
Many alerts are based on the dog noticing small changes from a person’s baseline—subtle shifts in breathing, posture, scent, or movement patterns. Regardless of the exact cue, the alert is most useful when it triggers a consistent response plan. Think of it as an extra nudge to check in with your body, not a replacement for medical monitoring or professional care.

The most effective cardiac-alert partnerships tend to be practical and repetitive. When an alert happens, the handler responds the same way as often as possible—because that pattern builds clarity for both human and dog. In busy environments, predictable steps also reduce decision fatigue: you don’t have to guess what to do when symptoms rise; you follow the plan.
Cardiac alert dogs can be trained for a mix of alert and response behaviors. Some teams focus on early warning—so the handler can sit or brace before dizziness peaks. Others emphasize “what happens next,” such as fetching medication, bringing a phone, or finding another person for help. Many handlers use a blended task list that covers both.
Medical alert/response dogs are widely recognized for their ability to alert to physiological changes and support response behaviors that may reduce risk during episodes, such as warning before blackouts and helping the handler take safety steps (source).
In real life, these tasks succeed because they’re built around habits. For example, a “retrieve meds” cue is far more dependable when the medication pouch always stays in the same place and the dog practices the skill during calm moments, not only during emergencies. The same is true for help-seeking: the dog needs a clear target person, a clear way to get their attention, and a clear return path to the handler.
“ "My dog’s alert gives me a head start. Even a minute is enough to sit down, drink water, and avoid pushing through symptoms." – Service dog handler”
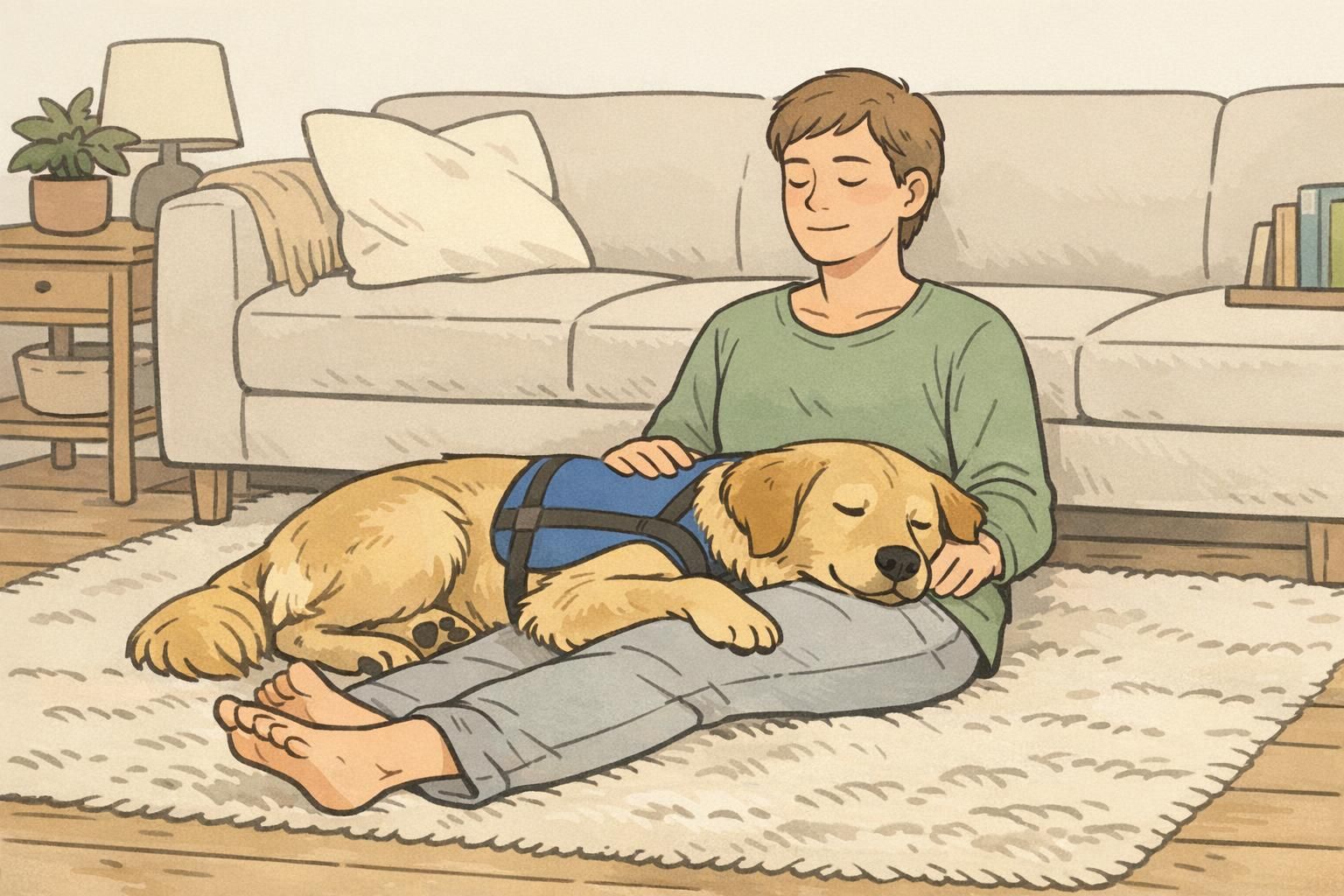
Beyond alerts, many cardiac alert teams use stability and comfort tasks to ride out symptom flares. One of the most well-known is deep pressure therapy (DPT). In everyday terms, DPT is when a dog applies calm, steady weight across the handler’s legs or lap (or leans in with controlled pressure) to support relaxation, grounding, and steadiness.
When symptoms like dizziness, shakiness, or adrenaline surges show up, it can be hard to slow down. DPT can help some handlers settle their breathing, stay oriented, and avoid panicking while they follow their care plan. It’s not a replacement for medical treatment—think of it as supportive care that pairs well with clinician-recommended steps.
For people who deal with dizziness or fainting risk, fall prevention is one of the most practical benefits of a cardiac alert dog. An early alert can give you time to sit, brace, or move away from hazards before you feel unsteady. Response behaviors can also help you make safer choices during transitions—standing up, stepping off a curb, or walking through a crowded aisle.
In the home, this can look like a dog signaling near the hallway, prompting the handler to sit on a bench before continuing. In public, it may be the dog prompting the handler to stop and find a stable surface, or guiding them toward a quieter area where they can recover.
Practical planning helps, too. Many handlers choose routes with predictable rest points, avoid long standing lines when possible, and make “stop spots” part of the routine. The more you plan for pauses, the less disruptive an alert feels—and the easier it is to respond quickly without drawing attention.
A cardiac alert dog’s value often goes beyond the task list. For many handlers, the biggest day-to-day change is independence—being able to run errands, attend class, or go to work with more confidence. When you trust your routine and your dog’s patterns, you may feel less pressure to “push through” symptoms alone.
Families and partners often feel benefits, too. When a dog can alert, retrieve a phone, or seek help, it can reduce the constant worry that something will happen unnoticed. This can be especially meaningful in households where a caregiver can’t be present every moment.
“ "It’s not that I never have symptoms. It’s that I feel like I have a teammate who helps me slow down and stay safe." – Service dog handler”
Cardiac alert work is specialized. Training often takes significant time, and the path looks different for every team. Some dogs naturally notice small changes and need structure to turn that into a clear alert. Other dogs excel at response tasks (like retrieving items or finding a person) and may be less consistent with early detection.
It’s also important to understand limitations. Detection is not guaranteed, and no dog should be treated as a sole safeguard. A cardiac alert dog is best used as part of a bigger safety plan that includes medical guidance, practical precautions, and a response routine you can follow even on hard days.
No. Many handlers find alerts and response behaviors helpful, but consistency can vary by dog, environment, and the handler’s symptoms. It’s best to view alerts as added support rather than a guarantee.
Yes. Response tasks—like guiding you to sit, retrieving a phone or medication, or getting help—can still add meaningful safety and confidence in daily life.
Usually not. Most teams do best with refreshers, real-world practice, and routine adjustments as health needs or daily schedules change.
In real life, service dog handlers often navigate quick questions in public—at stores, appointments, ride-shares, and during travel. Clear identification and simple informational materials can reduce friction and help interactions stay calm and respectful. Many handlers choose to carry optional registration details, ID cards, or certificates because it keeps information consistent and easy to share when questions come up.
These tools are best viewed as practical conveniences: they can help you communicate clearly, avoid repeating yourself, and feel more confident during everyday interactions. Different handlers prefer different setups—some like a digital option they can pull up quickly, while others prefer a printed card they can hand over without a long conversation.

Travel days and long outings can be more demanding on the body—more walking, more standing, less predictable meals, and less access to quiet recovery spaces. Planning ahead helps your cardiac alert dog work effectively, and it helps you feel more secure if symptoms start to rise.
It can help to build a “travel rhythm” that stays as close as possible to your normal routine: hydration, snacks (if that’s part of your plan), scheduled breaks, and quick access to medications. Many handlers also identify quiet places ahead of time—like a less crowded corner of an airport, a hotel lobby seating area, or a bench near the entrance of a venue.
For more planning ideas, see travel tips for going out with a service dog.

Some handlers also like having travel-ready identification and ADA-friendly educational materials packed in the same place every time. If that fits your lifestyle, consider a travel-ready service dog registration package for smoother trips.
If you want optional documentation to make day-to-day interactions simpler, it helps to choose a format that matches how you actually live. The best option is the one you’ll consistently carry and use—whether that’s a digital profile you can pull up quickly, a printed ID card that lives in your wallet, or a complete set that covers frequent travel and housing conversations.
If you’re building your everyday setup, a starter registration package for everyday identification can be a simple way to keep your dog’s details consistent and easy to access.
Small, repeatable habits can make cardiac alert support feel steadier and more predictable. The checklist below is designed to be practical: it focuses on what you can set up today, then refine over time based on what works for your body, your environment, and your dog.

For calm, clear communication in public settings, some handlers keep small informational cards ready to share when needed. If you’d like an easy option to carry, consider ADA law handout cards for calm, clear communication.